Why are All-on-1 dental implants more expensive than dentures?
Ever wondered why All-on-1 dental implants cost more than dentures?
Understanding the reasons behind this price difference can help you make informed choices about your oral health and long-term investment in a confident smile. In this comprehensive guide, you'll learn precisely what goes into the price tag for these two popular tooth replacement methods. We'll explore cost breakdowns, the impact of advanced technology, surgical complexity, material differences, and what all this means for your smile, comfort, and wallet over the long run.
Ever Wondered Why All-on-1 Dental Implants Cost More Than Dentures?
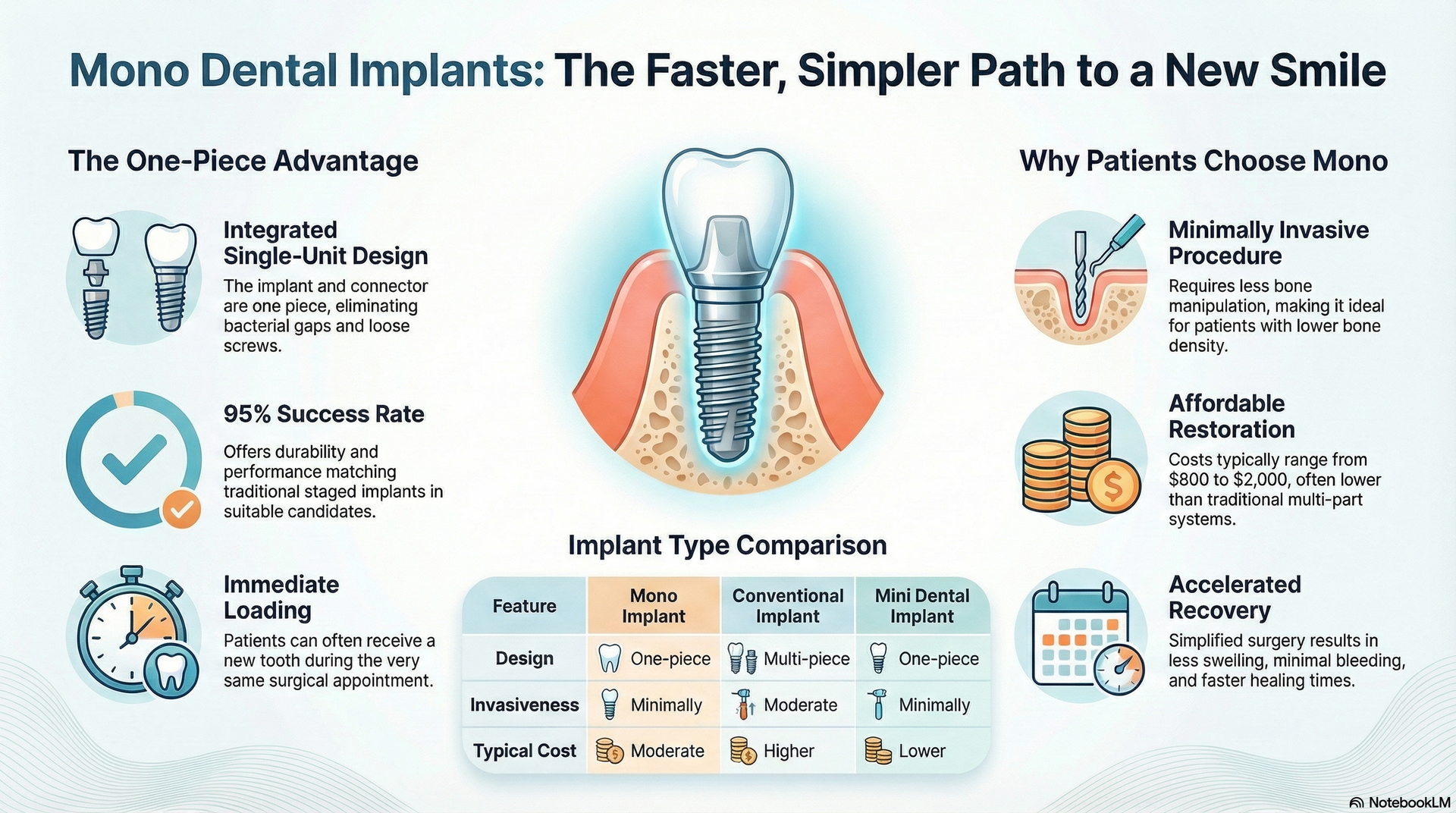
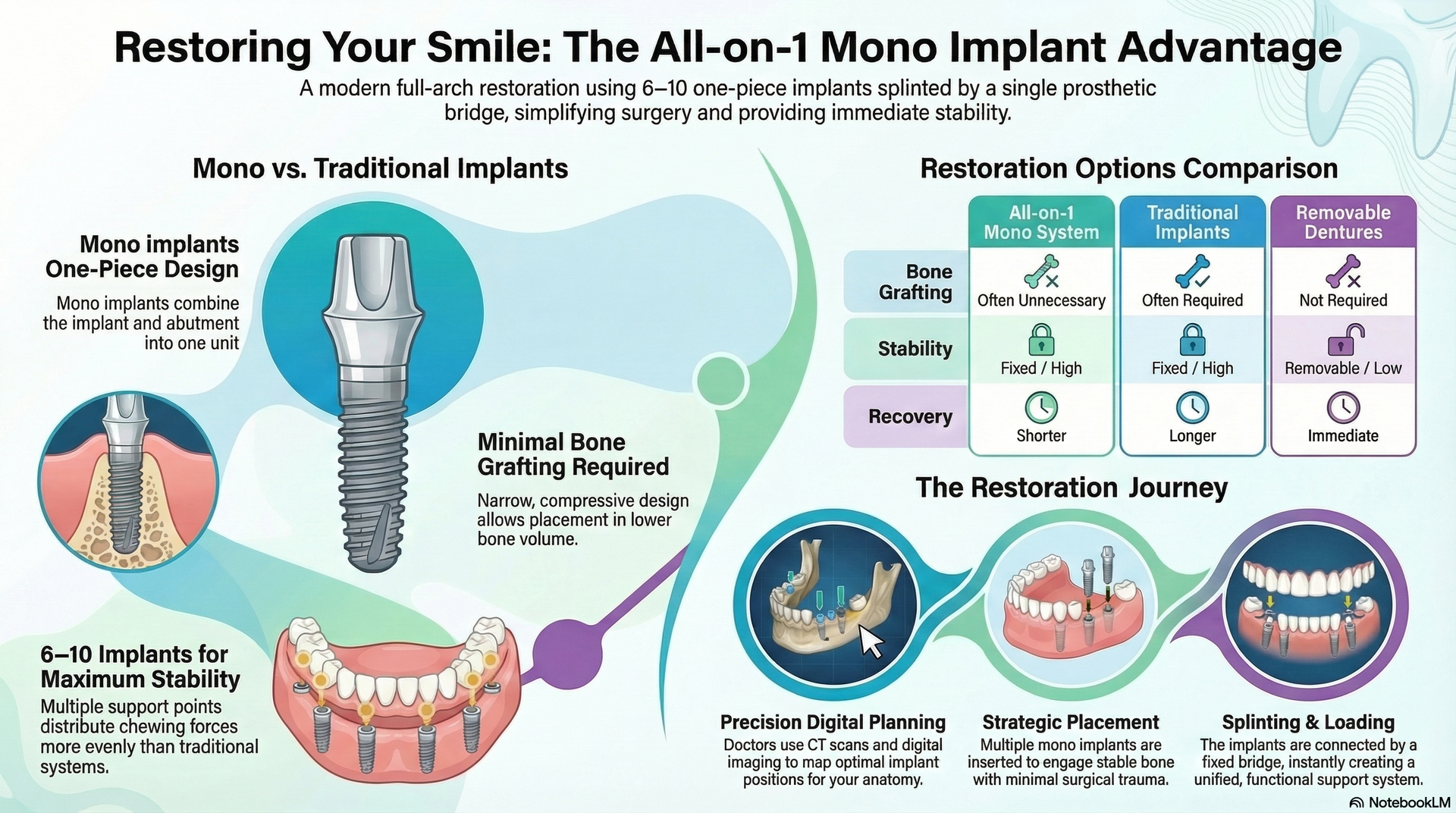
When considering your options for replacing missing teeth, it's natural to compare the cost of implant dentures—such as the innovative All-on-1 system—to traditional dentures. Many patients experience sticker shock when hearing the upfront cost of dental implants. But why do these solutions have a much higher initial investment? The answer lies in several key factors: the surgical expertise required, the quality of the materials used, the underlying dental technology, and the long-term benefits for your oral health and daily life. Unlike traditional dentures, which are mass-produced and offer a “quick fix,” All-on-1 implant denture solutions are tailored to each patient and involve advanced planning and procedures, which add to their price tag.
All-on-1 dental implants are designed to be a permanent solution. Their functionality, ability to prevent bone loss, and resemblance to natural teeth represent a dramatic improvement over removable dentures. While the cost of implant dentures may seem daunting at first, a deeper look reveals these expenses include more than just the prosthetic itself—they reflect investment in your long-term health, comfort, and confidence. Let's dig deeper into the core reasons for the cost difference between implant dentures and traditional dentures.
Understanding the Cost Difference: All-on-1 Dental Implants vs Dentures
The cost of implant dentures reflects not only the product you see but also the extensive behind-the-scenes work and technology involved. Traditional dentures may be fitted within weeks and require fewer dental visits, while All-on-1 dental implants involve specialized imaging, custom surgical guides, and placement of titanium implants in your jaw to serve as new tooth roots. The process can take several months and requires greater customization and skill, further increasing treatment costs. The strength, stability, and functionality of implants explain why many patients are willing to move beyond the upfront cost for longer-lasting value and peace of mind.
Understanding why all-on-1 dental implants are more expensive than dentures means appreciating both tangible and intangible benefits, such as improved chewing ability, enhanced confidence, and prevention of bone loss. The following sections break down the core reasons and explore which solution best matches your health needs and lifestyle.
What You’ll Learn About Why All-on-1 Dental Implants Are More Expensive Than Dentures
- The cost breakdown for All-on-1 dental implants and dentures
- Key contributing factors to price differences
- The role of dental implant technology, surgical expertise, and materials
- Long-term benefits versus upfront cost
- Patient considerations for oral health and financial planning
Cost of Implant: Breaking Down All-on-1 Dental Implants and Dentures
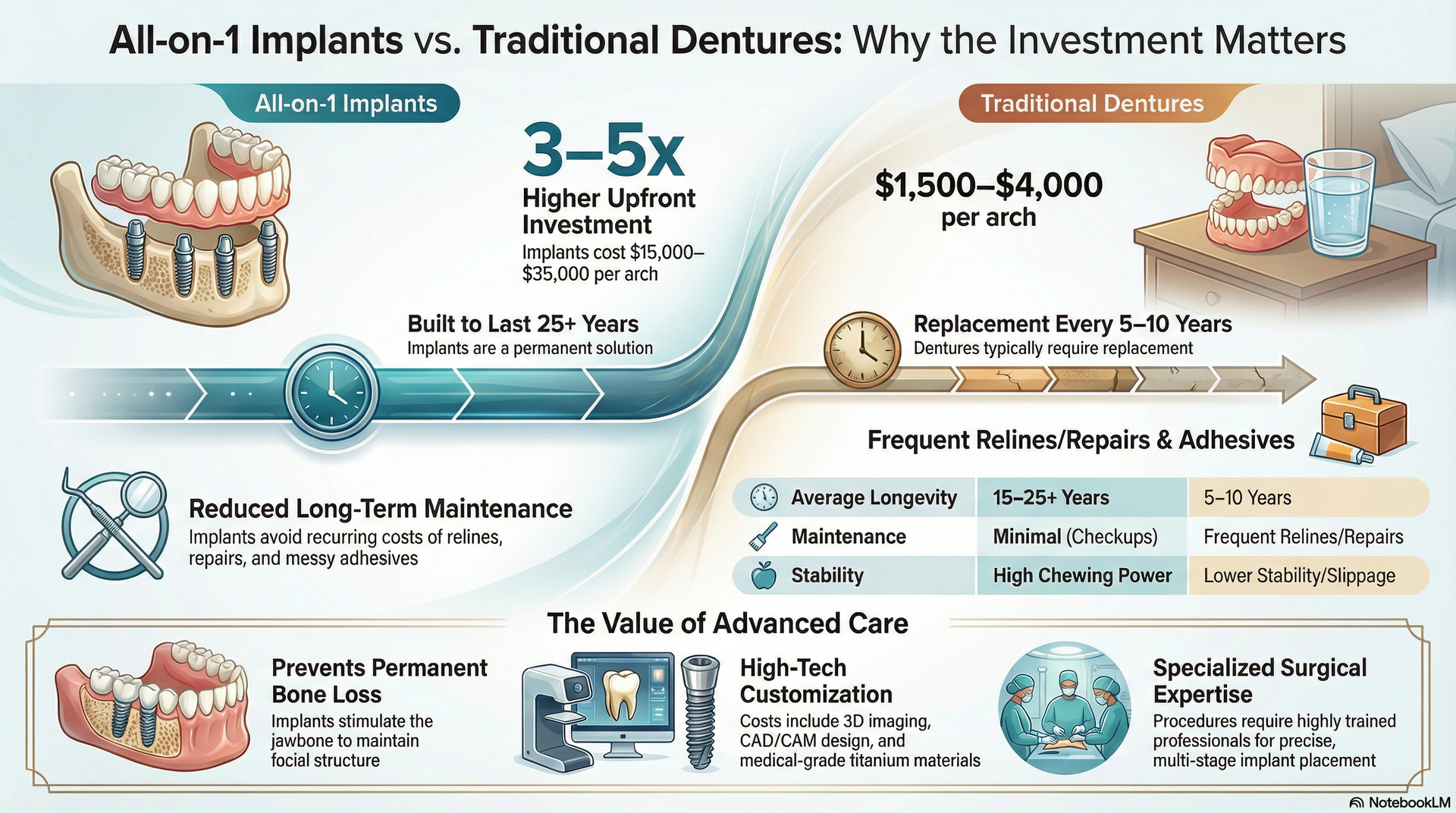
To better understand the financial implications, let’s compare the major costs of implant dentures and traditional dentures, element by element. The upfront cost of dental implants is generally 3–5 times higher than conventional dentures, but maintenance, longevity, and long-term oral health must also be considered. While traditional dentures are more cost-effective initially, they may require relining, repair, or full replacement every 5–10 years and can lead to jawbone changes due to bone loss.
All-on-1 dental implants, though expensive up front, are made to last decades. They anchor directly to your jawbone, support bone density, and are custom-designed for natural function and aesthetics. Although the investment is significant, implant dentures often reduce the need for ongoing repairs or adjustments. Let’s look at a side-by-side breakdown.
Comparison of Upfront Cost, Maintenance, and Longevity: All-on-1 Dental Implants vs Dentures
| Feature | All-on-1 Dental Implants | Traditional Dentures |
|---|---|---|
| Average Upfront Cost (Full Mouth) | $15,000–$35,000 per arch | $1,500–$4,000 per arch |
| Maintenance Costs | Minimal (regular dental checkups) | Frequent relines, repairs, and adhesives |
| Longevity | 15–25+ years | 5–10 years before replacement |
| Functionality | Very stable, high chewing power | Lower stability, reduced chewing power |
| Impact on Bone Loss | Helps prevent bone loss | Does not prevent bone loss |
Dental Implant Procedure: Why Complexity Drives Up Price
The process of receiving All-on-1 dental implants is complex and involves multi-stage planning, advanced surgical techniques, and advanced materials—each step adding to the cost of implant dentures. Let’s clarify how this complexity drives higher treatment costs and why so many patients believe the results are worth the investment. Unlike traditional denture fittings, which rely primarily on impressions and a dental laboratory, implant procedures require careful diagnostics, precise placement, and integration with your body.
Dental implants are not mass-produced solutions; each component, from the titanium posts to the custom prosthetic teeth, is designed to fit your unique oral anatomy. This ensures both functionality and aesthetics, but also entails higher production and labor costs. Furthermore, dental implant surgery must be performed by experienced professionals trained in implantology or prosthodontics, which increases the cost of implant dentures.
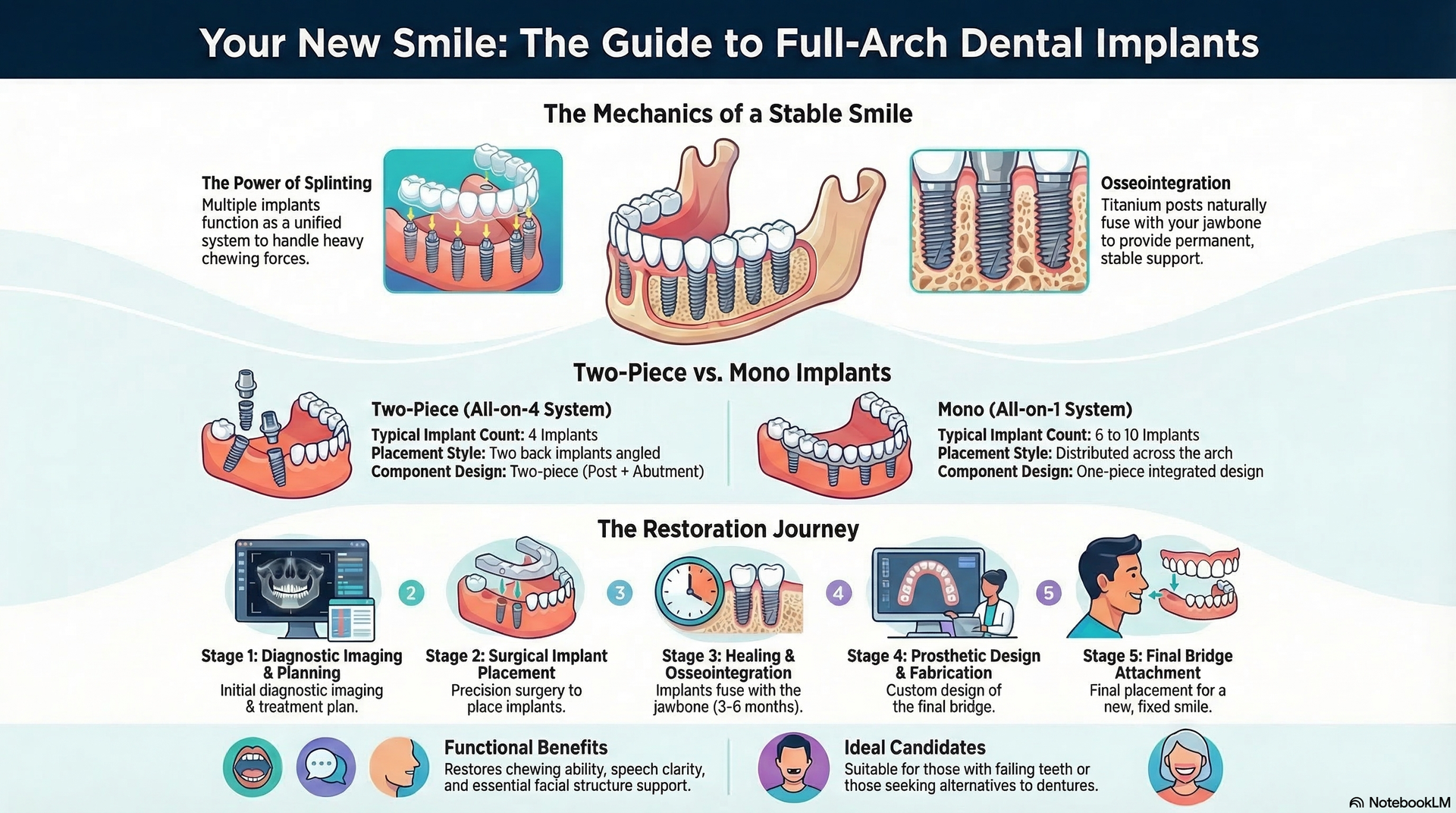
Surgical Steps in All-on-1 Dental Implants
Receiving All-on-1 dental implants involves more than simply attaching dentures to your gums. The process starts with a thorough diagnostic workup: 3D scans, bone analysis, and digital planning to determine the optimal number of implants for stability, usually four per arch. On surgery day, titanium implants are precisely placed into the jawbone, sometimes requiring bone grafting if the bone is insufficient. Following healing (osseointegration), custom prosthetic teeth are attached to the integrated implants, providing full function.
Each of these steps—diagnostics, implant placement, healing abutments, and prosthetic customization—requires specialized equipment and highly trained staff, which together contribute to the higher cost of all-on-1 dental implants compared with dentures. Ultimately, patients receive a permanent, stable, and life-changing result, but the process is time-intensive and resource-demanding.
Material Quality and Advanced Technology in Dental Implants
The price of All-on-1 implant dentures also reflects the advanced materials and digital technologies used. Implants themselves are typically made from medical-grade titanium, designed for biocompatibility and long-term support of your oral health. The artificial teeth may be fabricated from high-strength acrylics, advanced resin composites, or zirconia for maximum esthetics and durability.
Modern dental implant centers use CAD/CAM (computer-aided design and manufacturing), digital smile design, and 3D printing to ensure your prosthesis fits, functions, and looks just like natural teeth. This technology significantly improves comfort and outcomes but increases material and production costs compared with more traditional denture approaches. Such innovation means that implant dentures are not just a dental care product but an integrated investment in cutting-edge science and your quality of life.
Full Mouth Solutions: Comparing All-on-1 Dental Implants to Full Dentures
For patients missing all or most of their teeth, choosing between full-mouth dental implants and traditional dentures is a major life decision. The differences extend well beyond the initial bill. All-on-1 dental implants provide a full restoration of both appearance and function, securely anchoring your new smile for unrestricted eating and speaking. In contrast, even the best full dentures may slip or feel unstable during daily activities.
Patients need to weigh both financial and health considerations. All-on-1 dental implants are ideal for those seeking a long-term, hassle-free solution, offering stability, preventing bone loss, and a more natural experience. Full dentures may be appropriate for those seeking an affordable solution, though some loss of function and comfort is expected.
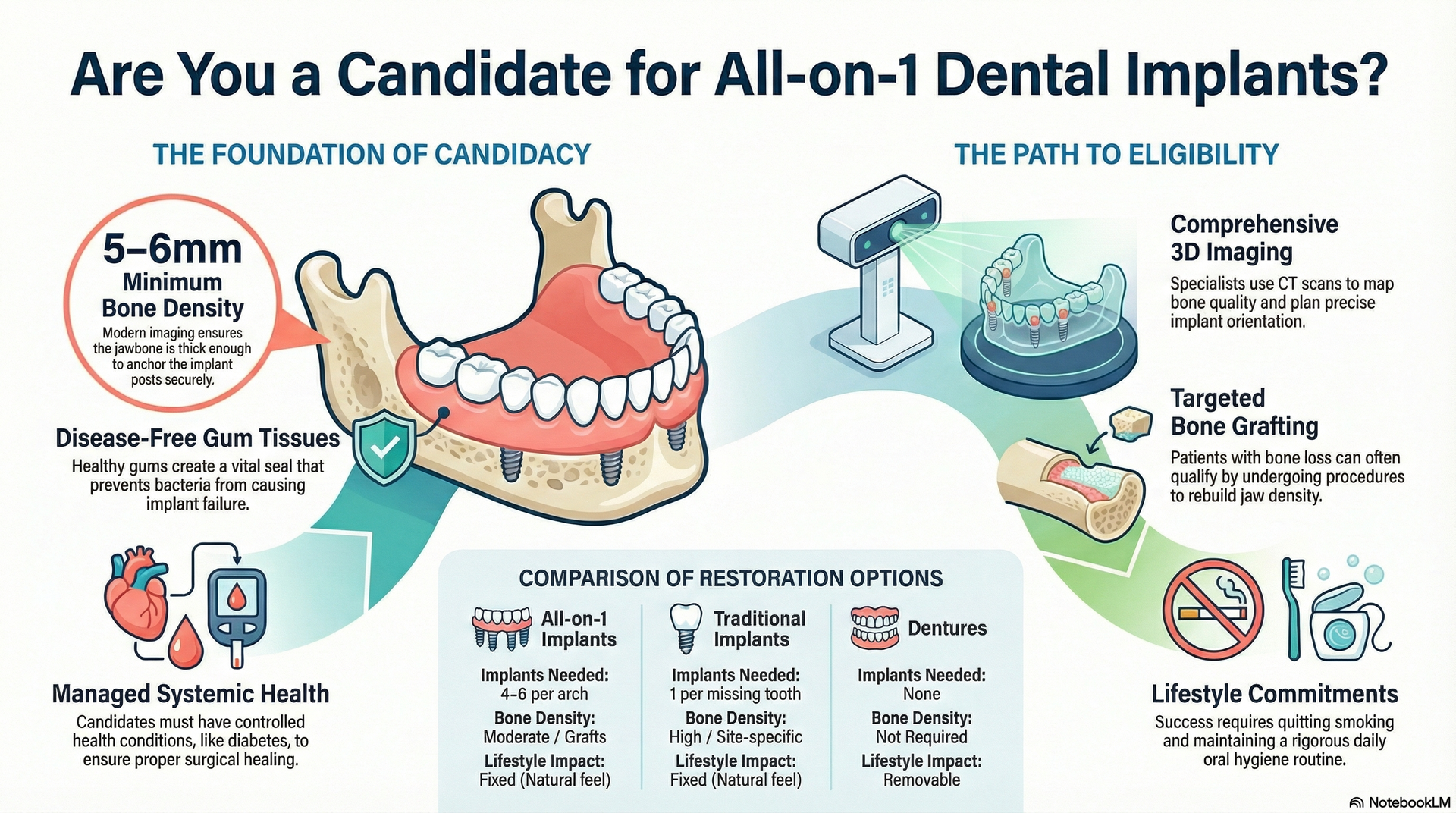
Who Is a Candidate for Full Mouth Dental Implants?
Full mouth dental implants are an advanced solution for patients with severe tooth loss, but not everyone is a candidate. Good systemic health, adequate bone density, and commitment to oral hygiene are prerequisites. Bone loss, which often follows years without teeth or with removable dentures, can affect candidacy—sometimes requiring bone grafting to restore the jaw before implants can be placed. The process involves a thorough evaluation, potentially with CBCT scans, to create a personalized plan for your mouth.
Patients who are tired of slipping dentures, want improved chewing ability, and are looking for a boost in self-esteem often find investing in full-mouth dental implants invaluable. Speaking with a dental implant specialist is the first step to discovering if All-on-1 implant denture treatment is right for you.
Implant-Supported Dentures vs Traditional Denture Solutions
It’s important to understand the difference between implant-supported dentures and traditional dentures. Implant-supported dentures—such as All-on-1—are anchored securely to implants embedded in your jawbone, whereas traditional dentures sit on top of the gums and may rely on suction or adhesives for retention. The added stability of implant dentures not only ensures a comfortable fit and restored chewing power, but also helps prevent bone loss by stimulating the jawbone as you eat and speak—something traditional dentures cannot provide.
Removable dentures can become loose over time as bone resorbs, leading to discomfort, speech difficulties, and loss of facial structure. Implant-supported dentures eliminate many of these issues, but cost more due to the surgery, planning, and materials required. Your dentist can help you explore your options and determine the best type of denture for your lifestyle, health, and finances.
Bone Grafting: Additional Costs and Considerations
Bone grafting, sometimes required before implant placement, is a surgical procedure in which natural or synthetic bone material is added to restore lost volume. This enables successful implant integration and improves long-term outcomes and stability. The need for bone grafting will raise your overall treatment cost and may require several months of healing before implant surgery can be completed.
Bone grafting costs vary depending on the extent of bone loss and the source of graft material. It’s a prime example of how treatment costs can vary based on your specific oral health condition. Discussing this in your consultation will help you anticipate both timeline and costs as you plan your dental implant journey.
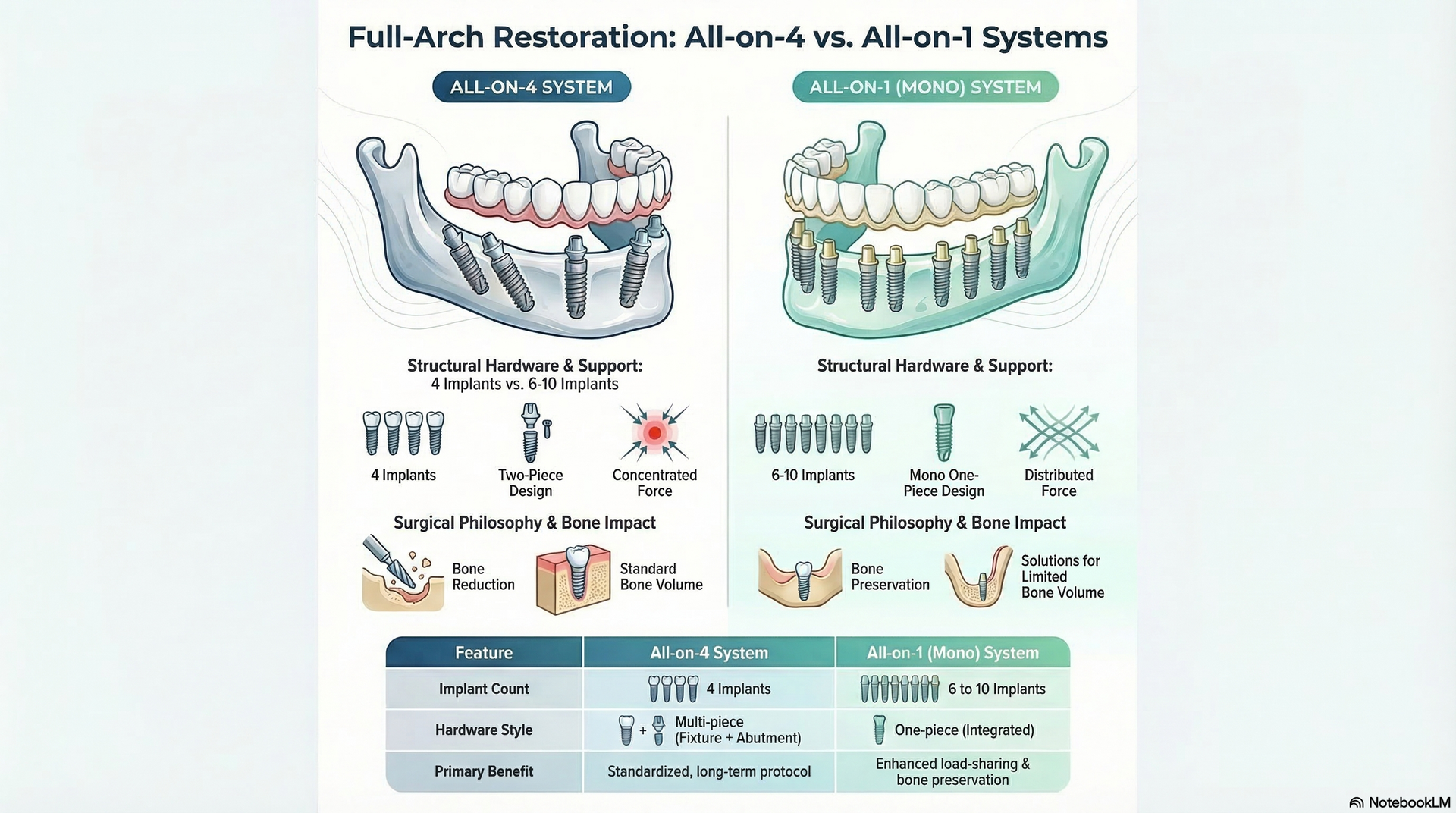
Number of Implants and Type of Denture Affecting Cost
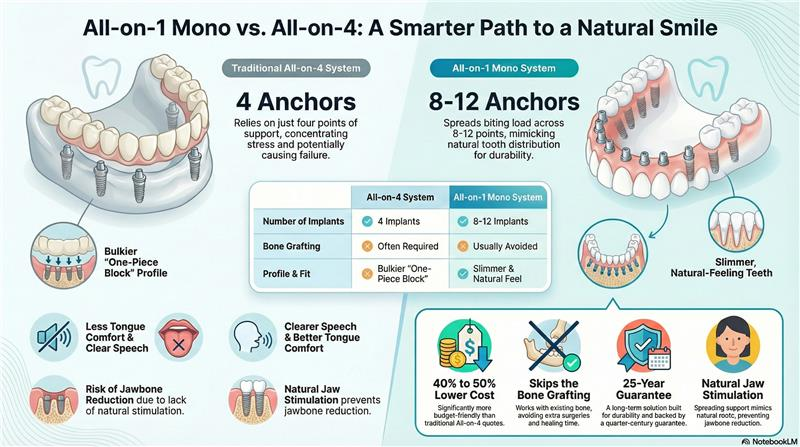
The total cost of implant dentures depends on the number of implants used and the type of prosthesis selected. All-on-1 typically uses four strategically placed implants per arch, while other solutions may use two to six or more implants. More implants generally provide greater stability but increase the upfront cost and procedural complexity. Meanwhile, the type of denture—fixed versus removable, premium materials versus standard—also affects both experience and overall cost.
How the Number of Implants Changes Upfront Cost
The upfront cost of your procedure is heavily influenced by the number of implants placed. All-on-1 and related “all-on-X” systems offer cost efficiency for full arches by minimizing the number of implants needed, while still providing stable, fixed support. Conversely, partial implant-supported dentures or cases requiring more implants (due to bone quality or a personalized fit) will require additional surgery, lab work, and components, further increasing treatment costs.
Fewer implants can reduce costs, but your dentist must ensure sufficient implants are used to maintain function and longevity. Financial planning and exploring financing options with your dental office can help you create a payment strategy that fits your needs. Discussing your payer coverage, such as dental insurance or Medicare Advantage plans, can help reduce out-of-pocket expenses for comprehensive oral health services.
Different Types of Denture and Dental Implant Approaches
Not all implant dentures are created equal. Some patients opt for removable dentures that snap onto implants for easier cleaning, while others prefer permanently fixed bridges for a seamless, lifelike smile. Variations exist not only in fit but also in aesthetic quality, material strength, and comfort. The type of denture you choose—traditional, implant-supported, or hybrid—will impact both functionality and your financial commitment.
Highly customized options, using top-tier materials and the latest technology, deliver the most natural results but cost more. Working with your dental team, you can tailor your implant denture treatment to your health, lifestyle, and budget, ensuring you receive the best possible outcome for your investment.
Upfront Cost vs Long-Term Investment: Cost of Implant Dentures
Choosing between All-on-1 dental implants and traditional dentures is about weighing upfront cost against a long-term investment in your oral health and daily well-being. Implants cost more initially, but many patients find that over time, the advantages in stability, function, bone health, and self-esteem far outweigh the upfront cost. Let’s break down what this means for your long-term wallet and quality of life.
Understanding Upfront Cost vs Maintenance and Replacement
The lower upfront cost of traditional dentures can be enticing, but ongoing costs must be factored in—such as relining, repairs, adhesives, and eventual replacement every 5–10 years. In contrast, dental implants, once integrated and properly maintained, can last decades. This means fewer dental visits and long-term savings. Evaluating both the short- and long-term financial implications of implant dentures will help you optimize your dental care investment.
Remember, proper dental care and regular check-ups are essential for maximizing the lifespan of your dental implants. A consultation with your dentist can provide personalized advice on anticipated maintenance and help ensure your treatment choice aligns with your overall health and financial goals.
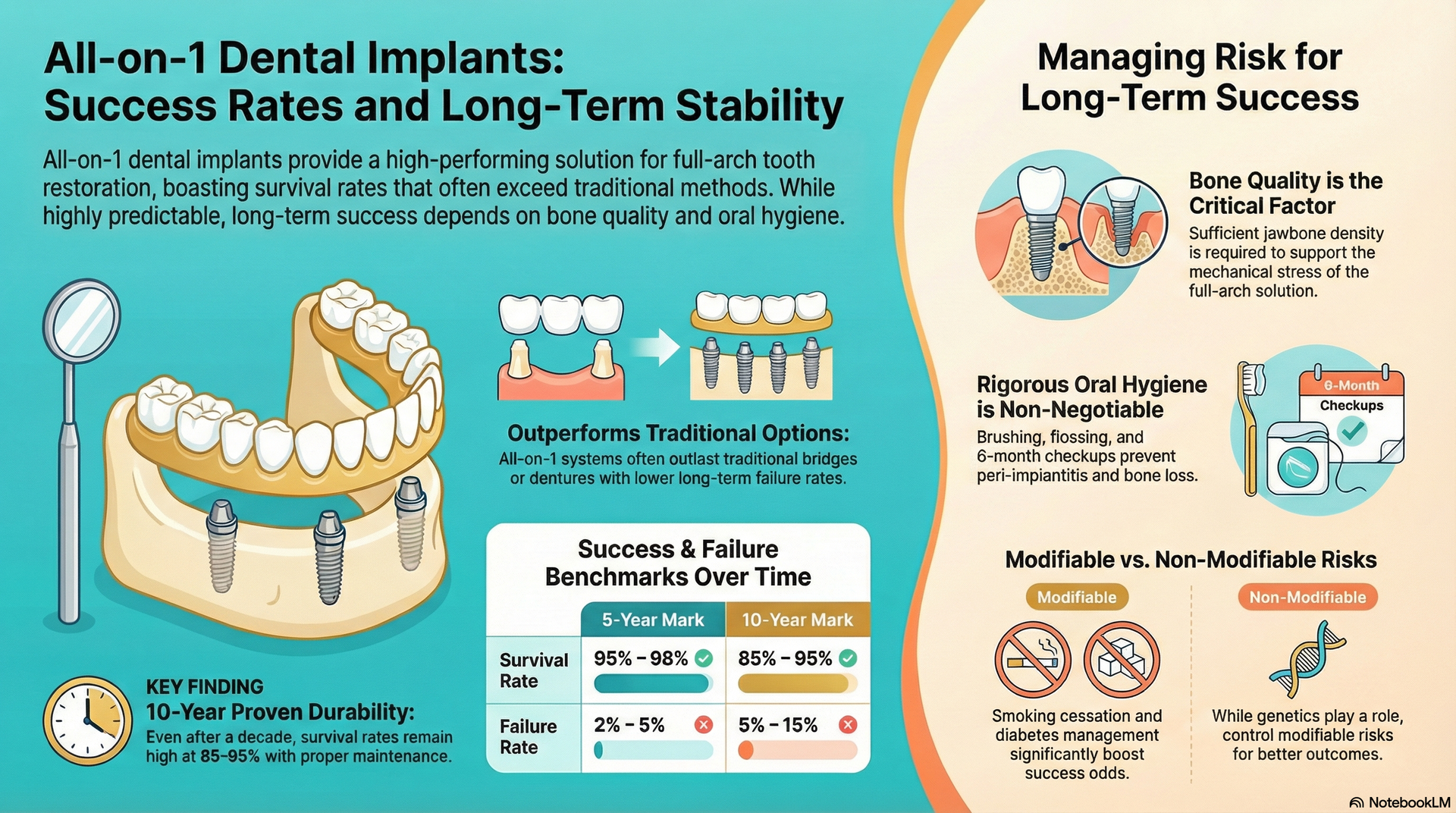
Longevity and Life Quality: Are Dental Implants Worth More?
Dental implants don’t just last longer—they help prevent bone loss, improve speech, allow unrestricted eating, and feel incredibly natural. This not only restores aesthetics but also bolsters confidence for social and professional interactions. For many, this boost in quality of daily life justifies the additional investment. As a leading prosthodontist puts it:
“Dental implants offer superior support and stability for lasting oral health, though the initial investment is higher than traditional dentures.” — Board Certified Prosthodontist
When comparing total value, the ability of implant dentures to maintain a vibrant, stable smile may outweigh their higher upfront cost—making them a worthwhile consideration for patients seeking durable, hassle-free solutions.
Risks and Benefits: Why Patients Choose All-on-1 Dental Implants Over Dentures
- Improved stability and chewing power
- Prevention of bone loss
- Enhanced speech and appearance
- Greater convenience compared to dentures
While every dental procedure carries some risk, the benefits of All-on-1 dental implants—when planned and placed by experienced professionals—routinely transform lives. Strong, fixed teeth restore freedom and comfort while supporting healthier jawbones and fresher breath. Patients often report greater self-assurance and spontaneity, secure in their new smiles.
Frequently Asked Questions About Why All-on-1 Dental Implants Are More Expensive
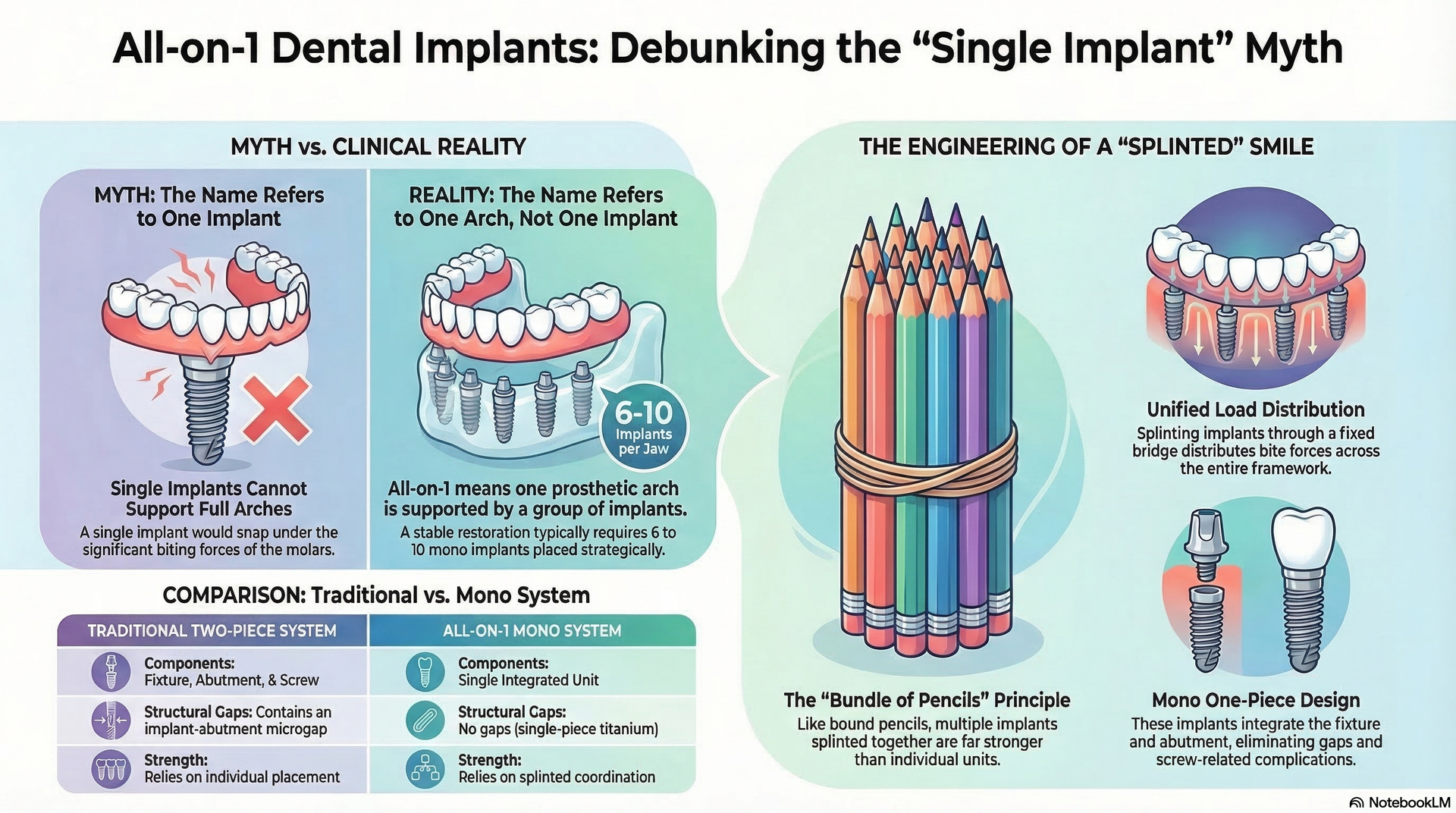
Why is a single dental implant so expensive?
Answer: A single dental implant is costly due to the surgical procedure, high-grade materials, custom prosthetics, and the expertise required. Each implant serves as a durable, fixed-tooth replacement, offering strength and longevity that are uncommon with traditional dentures.
Is it true that Medicare now pays for dental implants?
Answer: While Medicare typically does not cover dental implants, some Medicare Advantage plans may offer supplemental dental benefits. It's essential to verify coverage specifics with your insurance provider.
Are single tooth implants better than dentures?
Answer: Single tooth implants provide greater functionality, stability, and bone preservation compared to dentures, but at a higher cost. The best solution depends on your specific oral health needs and budget.
What does no one tell you about dental implants?
Answer: Dental implants require surgical treatment and a healthy jawbone. While their upfront cost is higher, they deliver lasting benefits, including bone preservation, comfort, and natural aesthetics. There may also be a significant healing period.
Key Takeaways: Summing Up Why All-on-1 Dental Implants Cost More Than Dentures
- Initial investment for dental implants is higher due to surgical expertise, material quality, and customization
- Dentures incur lower upfront costs but may require ongoing repairs or replacement
- Dental implants help prevent bone loss, improving long-term oral health
- All-on-1 dental implants offer a more permanent, stable, and natural-feeling solution
“Investing in dental implants today can save time, money, and anxiety over the course of a lifetime.” — Brian Carter, DDS
Ready to Learn More? Call for a Free Consultation and X-ray (616) 681-5506
Take the first step toward a confident, lasting smile. Explore your options with a dental implant specialist—call today for a complimentary consultation and digital X-ray!
Sources
Recent Posts