What’s the failure rate of All-on-1 implants?
Wondering how often All-on-1 implants fail? Understanding their failure rate can help you make informed choices for a confident smile. Are these dental implants the right solution for you? Let’s explore the facts together and uncover what you need to know before deciding.
Introduction: Understanding the Failure Rate of All-on-1 Implants
- Wondering how often All-on-1 implants fail? Understanding their failure rate can help you make informed choices for a confident smile. Are these dental implants the right solution for you? Let's explore the facts together and uncover what you need to know before deciding.
- Learn what the term 'failure rate' means in the context of All-on-1 dental implant procedures.
- Formal definition of implant failure, dental implant failure, and survival rate.
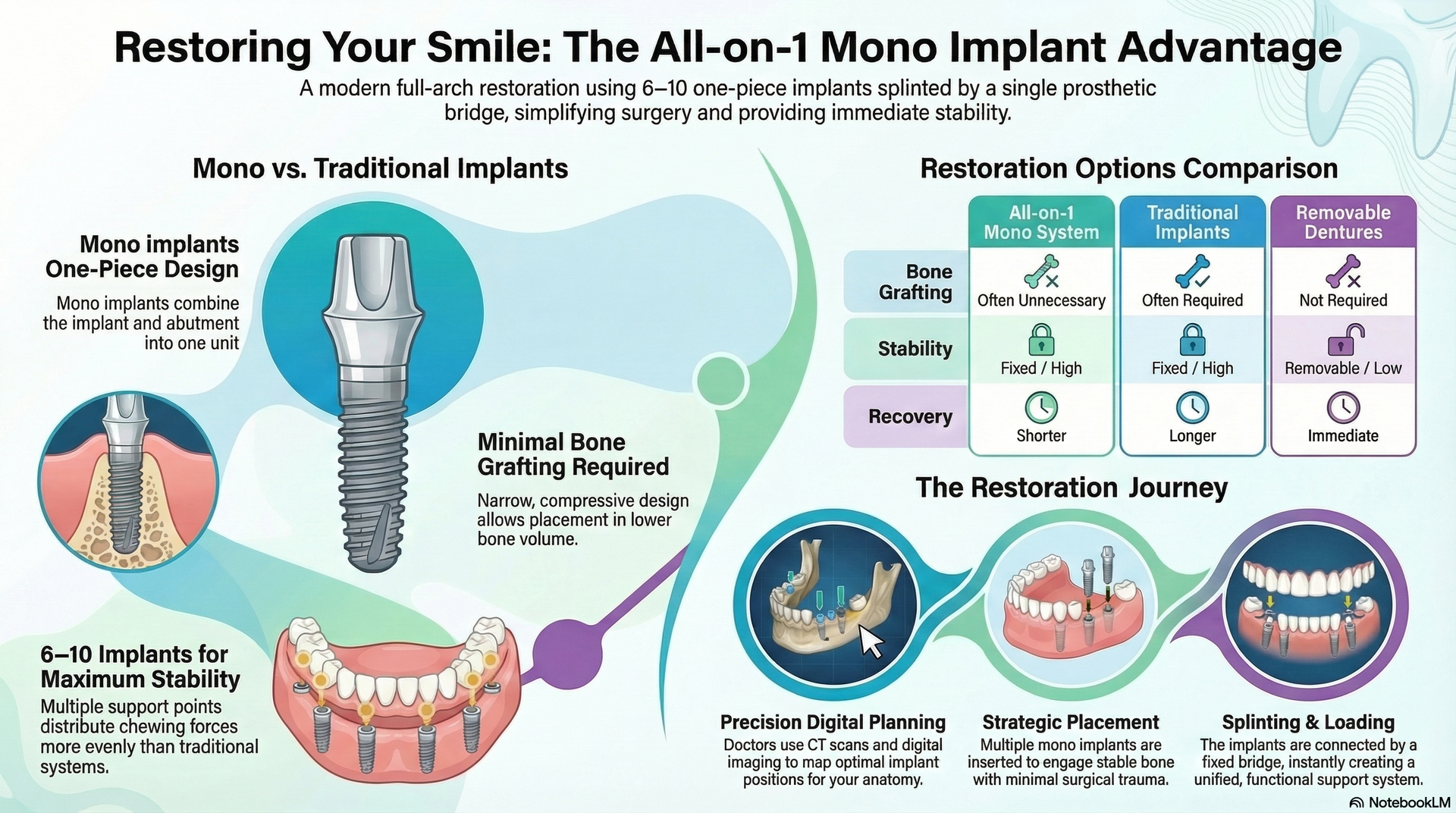
In dental restoration, few options are as transformative as the All-on-1 implant system. But before deciding if this advanced procedure is right for you, it’s essential to address a critical consideration: what’s the failure rate of All-on-1 implants? In this article, we’ll break down what “failure rate” means in the context of dental implants and how it compares to concepts like “success rate” and “survival rate. ” Knowing these statistics allows you to make more confident choices for your oral health.
Implant failure typically refers to any situation in which a dental implant does not integrate successfully with the bone, becomes loose, or must be removed due to complications. The survival rate, meanwhile, indicates the percentage of implants still functioning over a set period, such as five or ten years. Understanding these definitions is the foundation for evaluating the real-world performance of All-on-1 dental implants.
What You’ll Learn About All-on-1 Implant Failure Rate
- Key statistics about failure rates and survival rates of All-on-1 dental implants
- Risk factors and causes for implant failure
- How bone quality, bone grafting, and oral hygiene affect success
- What to expect if an implant fails and how to maximize your chances of success after an implant failure
By reading this article, you’ll discover not only key statistics regarding the failure and survival rates of All-on-1 implants, but also the main risk factors that increase the chance of implant failure. We’ll delve into the roles of bone quality, bone grafting, and oral hygiene in determining the success of your implants. Finally, we’ll explain how to identify signs of failure, what recovery may involve if things do go wrong, and the specific measures that significantly boost your odds of a healthy, enduring smile.
Overview of the Success Rate and Failure Rate of All-on-1 Implants
- Summary of current research and clinical data on the failure rate and success rate of All-on-1 dental implants
- Comparison of the survival rate and longevity of conventional dental implants
The failure rate of All-on-1 implants is exceptionally low, especially when compared to conventional dental implants. Clinical studies consistently show survival rates for All-on-1 systems of 95-98% at 5 years and 85-95% at 10 years, making them among the highest-performing solutions for full-arch tooth replacement. In contrast, conventional single dental implants have similar survival rates. Still, they may show slightly higher failure rates in certain complex cases, such as when multiple implants are placed in areas with suboptimal bone.
The success rate of All-on-1 implants is driven not only by improved implant designs and materials but also by advances in diagnostics, treatment planning, and patient selection. A recent study found that immediate-load protocols and careful avoidance of high-risk patients minimize late failure rates in All-on-1 systems. This translates to a high success rate and predictable outcomes for the vast majority of recipients. Importantly, a higher survival rate means that these implants can often outlast traditional bridges or dentures, making them a sound long-term investment in your oral health.
"All-on-1 implants represent a significant advancement in dental restoration, with clinical studies showing survival rates comparable to or better than traditional methods. " — Dr Jared Van Ittersum
| Implant Type | Failure Rate (5 Years) | Failure Rate (10 Years) | Survival Rate (5 Years) | Survival Rate (10 Years) | Comments |
|---|---|---|---|---|---|
| All-on-1 Dental Implants | 2–5% | 5–15% | 95–98% | 85–95% | High success rates with proper care and patient selection |
| Conventional Dental Implants | 2–6% | 5–20% | 94–97% | 80–95% | Similarity in survival rates; slightly higher late failures in complex cases |
Key Risk Factors Contributing to the Failure Rate of All-on-1 Implants
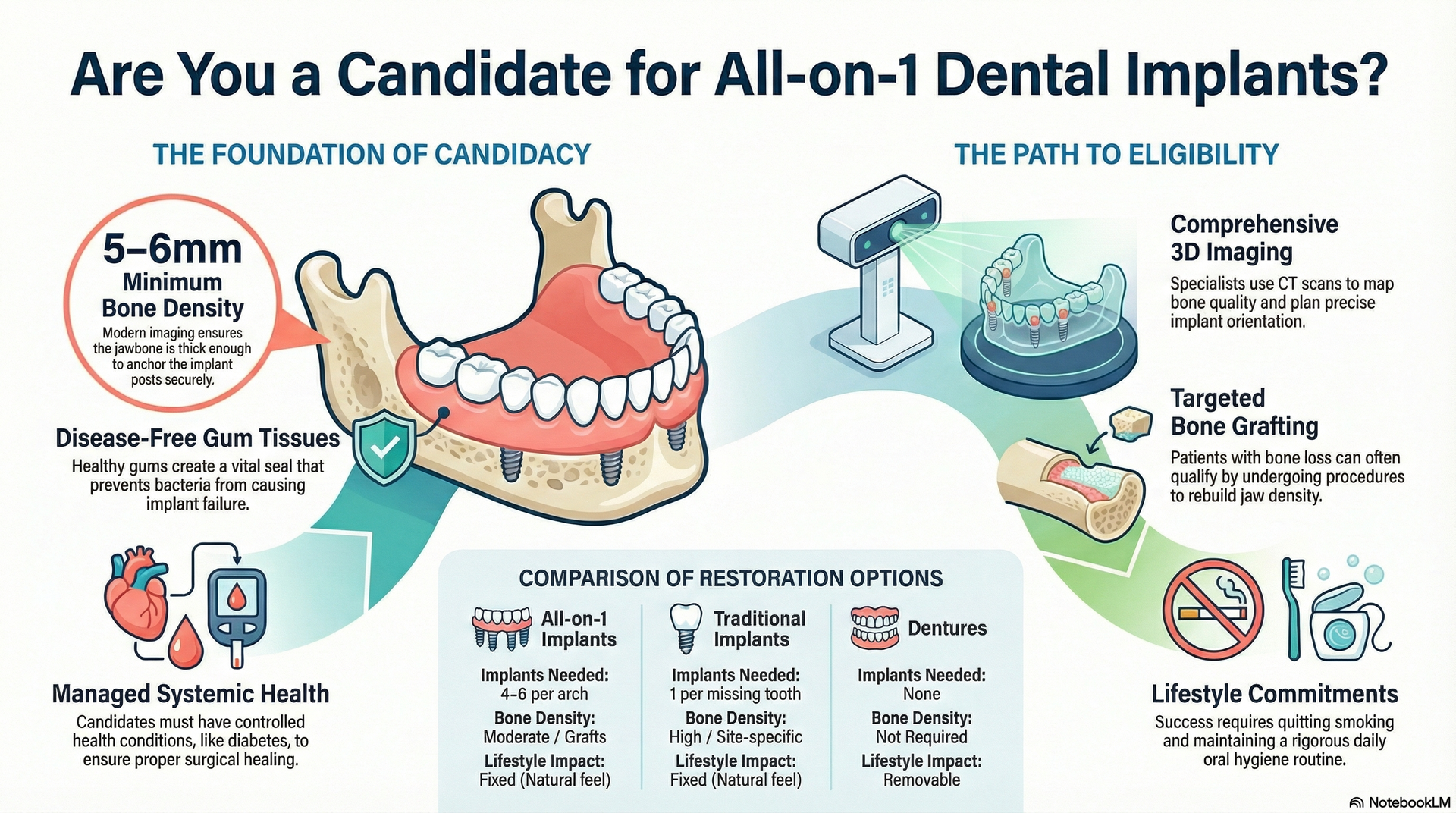
- Overview of common risk factors such as bone quality, systemic health, oral hygiene, and history of periodontal disease
- Discuss how bone grafts or bone grafting impact the failure rate.
- Breakdown of modifiable versus non-modifiable risk factors
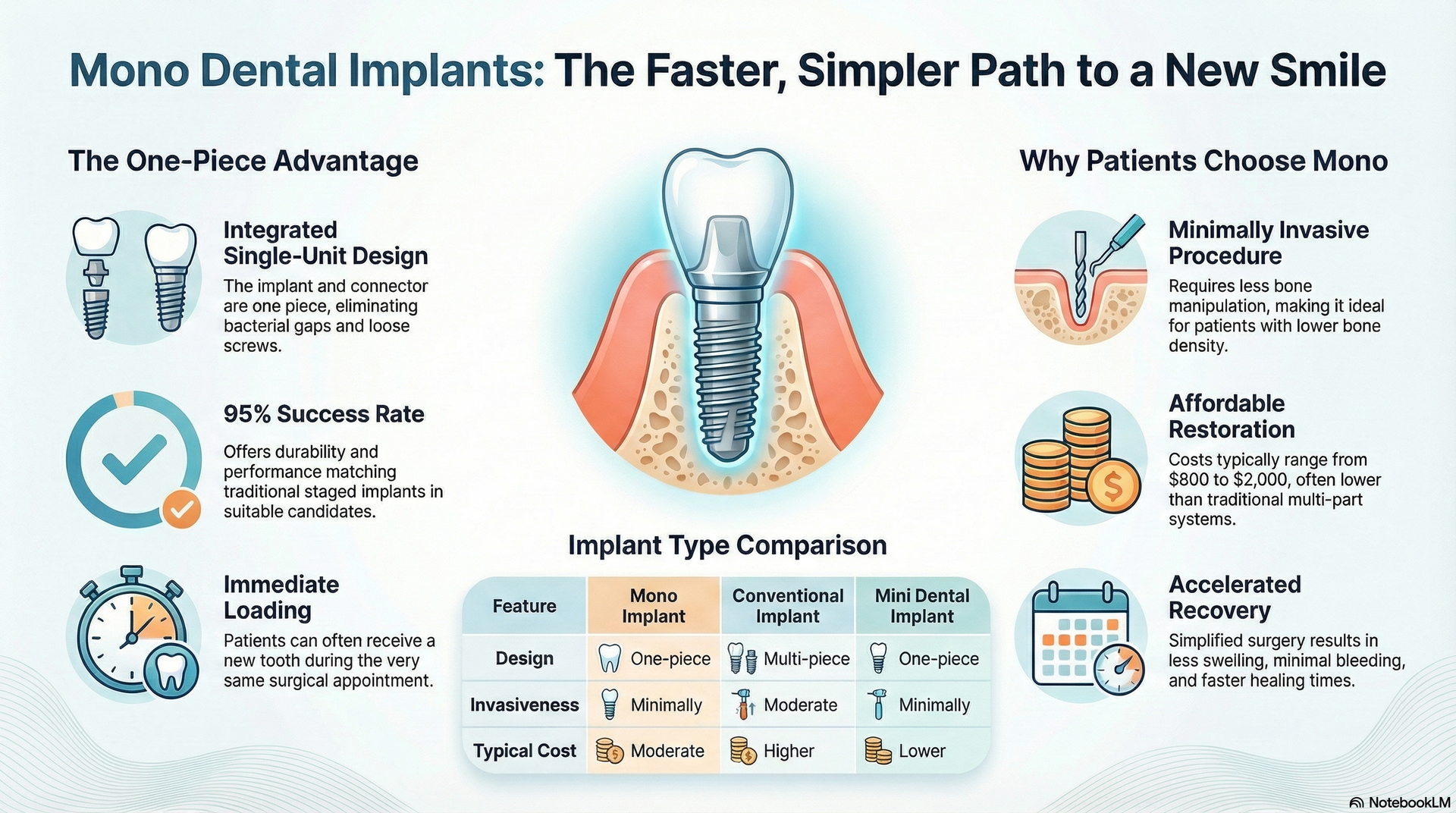
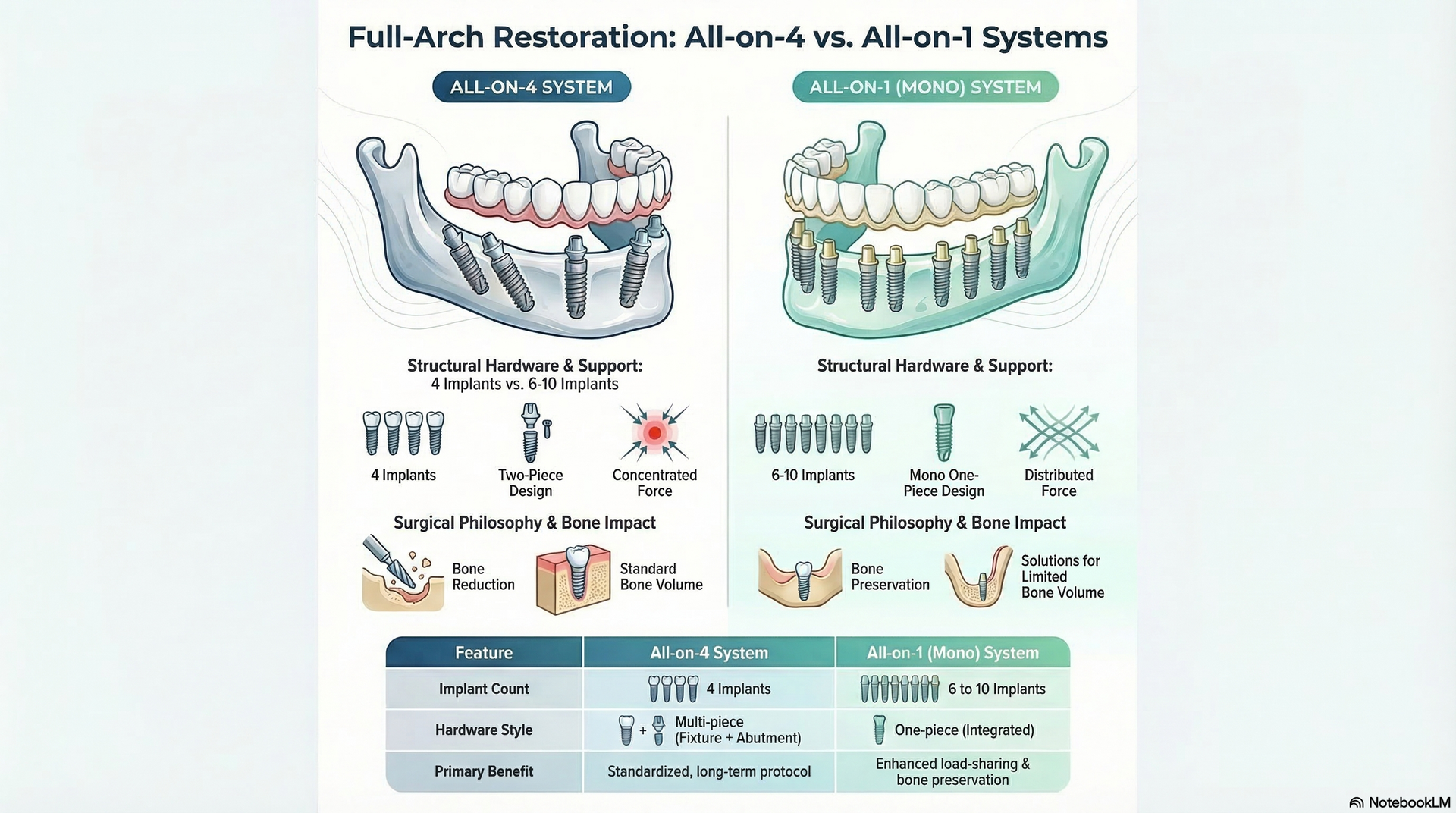
Although All-on-1 dental implants have a high success rate, certain factors can increase the risk of failure. The most important of these is bone quality. Because All-on-1 implants are anchored in the dense, outer layer of bone—which is significantly stronger than the softer inner marrow—they often provide excellent stability and rarely require bone grafting. In contrast, traditional two-piece implants are typically placed deeper into the softer interior bone, where grafting is more commonly needed to create adequate support.
In addition to bone quality, systemic conditions such as diabetes, smoking, osteoporosis, and immune disorders can affect healing and long-term success. A history of periodontal disease or poor oral hygiene habits can also increase the likelihood of complications following implant surgery.
Some risk factors are non-modifiable (like age or genetics). In contrast, others—such as oral hygiene habits, smoking cessation, and overall health maintenance—can be controlled or addressed in your treatment plan. Effective communication with your oral surgeon and a commitment to healthy habits will maximize your chances for long-term success and minimize the need for remedial dental intervention.
The Role of Bone Quality, Bone Graft, and Bone Grafting in Implant Failure
- How bone quality contributes to dental implant failure and affects the failure rate
- When bone graft or bone grafting is necessary for All-on-1 procedures, and its impact on the success rate
- Common complications related to bone graft procedures
Although All-in-1 implants are designed to engage the dense outer layer of bone and typically do not require grafting, there are occasional cases where bone grafts are still necessary. For this reason, choosing an experienced implant surgeon who can accurately assess bone quality and determine when grafting is truly needed is essential.
Bone quality remains one of the most significant factors influencing the success of All-in-1 implants. The jawbone must have adequate density and volume to withstand the mechanical demands of a full-arch restoration. If bone loss or structural deficiencies are present, a grafting procedure may be recommended to strengthen the area prior to implant placement.
Patients undergoing bone grafting should be aware that healing and bone integration can take several months. Regular follow-ups during this stage are essential. Proper planning and collaboration with an experienced oral surgery team are crucial for minimizing implant failures and late failure occurrences related to poor bone quality.
How Oral Hygiene Influences Implant Failure and Survival Rate
- Importance of exceptional oral hygiene after All-on-1 implant placement
- How poor oral hygiene increases implant failure risk and reduces survival rate
- List of best practices for oral hygiene to minimize failure rate
Maintaining excellent oral hygiene is non-negotiable for anyone with All-on-1 dental implants. Failure to keep the implant and gum tissue clean can lead to peri-implantitis—a form of gum inflammation that, if left untreated, leads to bone loss and eventual implant failure. Studies point to oral hygiene as one of the most significant modifiable risk factors; patients who brush and floss consistently, schedule regular dental visits, and avoid tobacco show substantially lower failure rates and higher survival rates.
- Use a soft-bristled toothbrush and non-abrasive toothpaste twice daily.
- Floss or use an interdental brush around the gum line and under the prosthesis
- Rinse with an antimicrobial mouthwash as recommended.
- Schedule professional cleanings and checkups every 6 months—or more frequently if advised.
- Immediately address any signs of gum redness, swelling, or discomfort
By sticking to these best practices, you drastically reduce your risk of implant failure and increase your chances of enjoying a beautiful, long-lasting smile.
Common Causes of Dental Implant Failure in All-on-1 Systems
- Review of the most frequent underlying causes of implant failure, including biological, mechanical, and patient factors
The causes of dental implant failure in All-on-1 systems can generally be grouped into three categories: biological (e.g., bone loss, infection), mechanical (e.g., prosthesis breakage, screw loosening), and patient-related factors (e.g., poor oral hygiene, smoking, systemic health problems). In the first weeks after implant surgery, insufficient bone integration is a common cause of early failure. Over time, peri-implantitis due to inadequate cleaning or chronic medical conditions can also jeopardize the implant’s stability.
Mechanical failures can result from issues with the prosthesis, excessive chewing force, or improper placement. Patient habits such as bruxism (teeth grinding) and failure to attend regular follow-up appointments increase risk. Early detection and proactive management of these factors are critical to avoiding late failures and ensuring a high survival rate.
| Cause | Frequency | Possible Prevention |
|---|---|---|
| Poor bone quality or volume | Common | Bone grafting/pre-surgical planning |
| Infection (peri-implantitis) | Low | Oral hygiene and professional care |
| Systemic diseases (diabetes, osteoporosis) | Moderate | Medical management, risk factor screening |
| Prosthesis breakage | Occasional | Proper design, maintenance, and prompt repairs |
| Poor oral hygiene or smoking | Common | Good habits, behavior modification |
Signs and Symptoms of All-on-1 Implant Failure
- Visual and clinical indicators of a failed implant
- How to distinguish between normal post-surgical symptoms and signs of dental implant failure
Recognizing the early signs of dental implant failure is essential for prompt intervention. Key indicators include persistent pain, noticeable prosthesis mobility, swelling, gum recession, bleeding, or purulent drainage around the implant site. While mild discomfort and swelling are normal after oral surgery, these should subside within a few days. If symptoms continue beyond 2–3 weeks or worsen, it could indicate a developing failure.
Other warning signs include a feeling that the implant “just doesn’t fit right,” difficulty chewing, or recurring bad breath. Dental professionals urge patients to monitor their healing process closely—and to report any concerns immediately for early investigation and management. Timely action can often save an implant before complete failure occurs.
"Early detection of implant failure is crucial. Patients should report persistent pain or mobility to their dental provider immediately. " — Dr Jared Van Ittersum
Diagnosis and Management of All-on-1 Implant Failure
- Diagnostic criteria and steps for confirming dental implant failure
- Outline of clinical interventions after implant failure
- What patients can expect if a failed implant needs replacement?
Diagnosing implant failure involves clinical examination and radiographic imaging to assess bone support, detect mobility, or identify infection. Dentists follow strict diagnostic protocols to determine whether an implant is salvageable through non-surgical or surgical intervention. Sometimes, treating local infection or adjusting the prosthesis prevents failure; in other instances, removal of the failed implant is necessary.
If implant replacement is required, patients can expect a healing period before placement of a new implant—often with additional bone grafting to rebuild lost tissue. The overall treatment plan may be extended, but with appropriate management and risk-factor modification, long-term restoration remains feasible for most patients.
How to Reduce the Failure Rate of All-on-1 Implants: Patient & Provider Tips
- Checklist for patients and providers to minimize risk factors
- Pre-treatment strategies, including evaluation of bone quality, consideration of bone grafting, and personalized treatment planning
- Lifestyle and post-operative guidelines to maximize the survival rate
- Importance of following up with your dental surgery team
Lowering the risk of implant failure in All-on-1 systems starts well before surgery, through comprehensive evaluation and planning, and continues throughout the recovery and maintenance phase. Providers should rigorously assess bone quality, medical history, and lifestyle habits. Patients should seek experienced specialists, follow all pre-operative instructions, and commit to maintaining oral and systemic health.
- Attend all scheduled consultations and planning visits.
- Address any health issues with your general practitioner.
- Discuss the pros and cons of bone grafting if the bone quality is low.
- Quit smoking and manage conditions like diabetes or osteoporosis proactively.
- Adhere to all postoperative oral hygiene and diet instructions.
- Report any unusual symptoms immediately to your dental provider
Routine follow-up care with your dental surgery team dramatically increases the lifetime of your All-on-1 implants, helping you achieve the high survival rates observed in clinical research.
- Embedded educational video summarizing the failure rate, survival rate, and success rate statistics for All-on-1 dental implants
Long-term Survival Rate of All-on-1 Dental Implants
- What clinical studies show about 5-year and 10-year survival rates
- How maintenance, risk factor management, and oral hygiene contribute to longevity
- Statistics comparing the survival rates of All-on-1 to individual dental implants
Recent clinical data strongly support the long-term durability of All-on-1 dental implants. Over five years, the survival rate consistently exceeds 95%. Even at the ten-year mark, most studies report survival rates of 85% and higher. These figures compare favorably with individual implants, despite higher initial loads and fewer anchor points for the prosthesis. The keys to this longevity are effective risk factor management, adherence to maintenance guidelines, and robust oral hygiene regimens.
Patients who schedule regular follow-ups, professionally clean their prosthesis, and address systemic health issues proactively are far more likely to enjoy long-term benefits. With proper care, All-on-1 implants can offer life-changing results for years—and often decades—after the initial placement.
Comparing All-on-1 Implant Failure Rates Internationally
- Review of global clinical studies: Where is the highest rate of implant failure?
- Regional, provider, and protocol variations influencing failure rates
International studies show regional variation in failure rates for All-on-1 implants, influenced by factors including access to specialist care, technological resources, and clinical protocols. For example, countries with robust dental training programs and rigorous regulations—such as the US, Canada, Germany, or Australia—consistently report low failure rates, reflecting global best practices.
Regions with limited access to qualified oral surgeons, or where less experienced providers perform these complex treatments, may see slightly higher failure rates. In general, proper provider selection and adherence to evidence-based protocols are far more critical than location alone—underscoring the importance of research and consultation, regardless of where. You choose to undergo All-on-1 implant restoration.
Financial Implications: Who Pays When a Dental Implant Fails?
- Breakdown of costs involved in handling implant failure
- Discuss insurance, warranties, and provider policies
- Tips for negotiating coverage or warranties for replacing failed implants
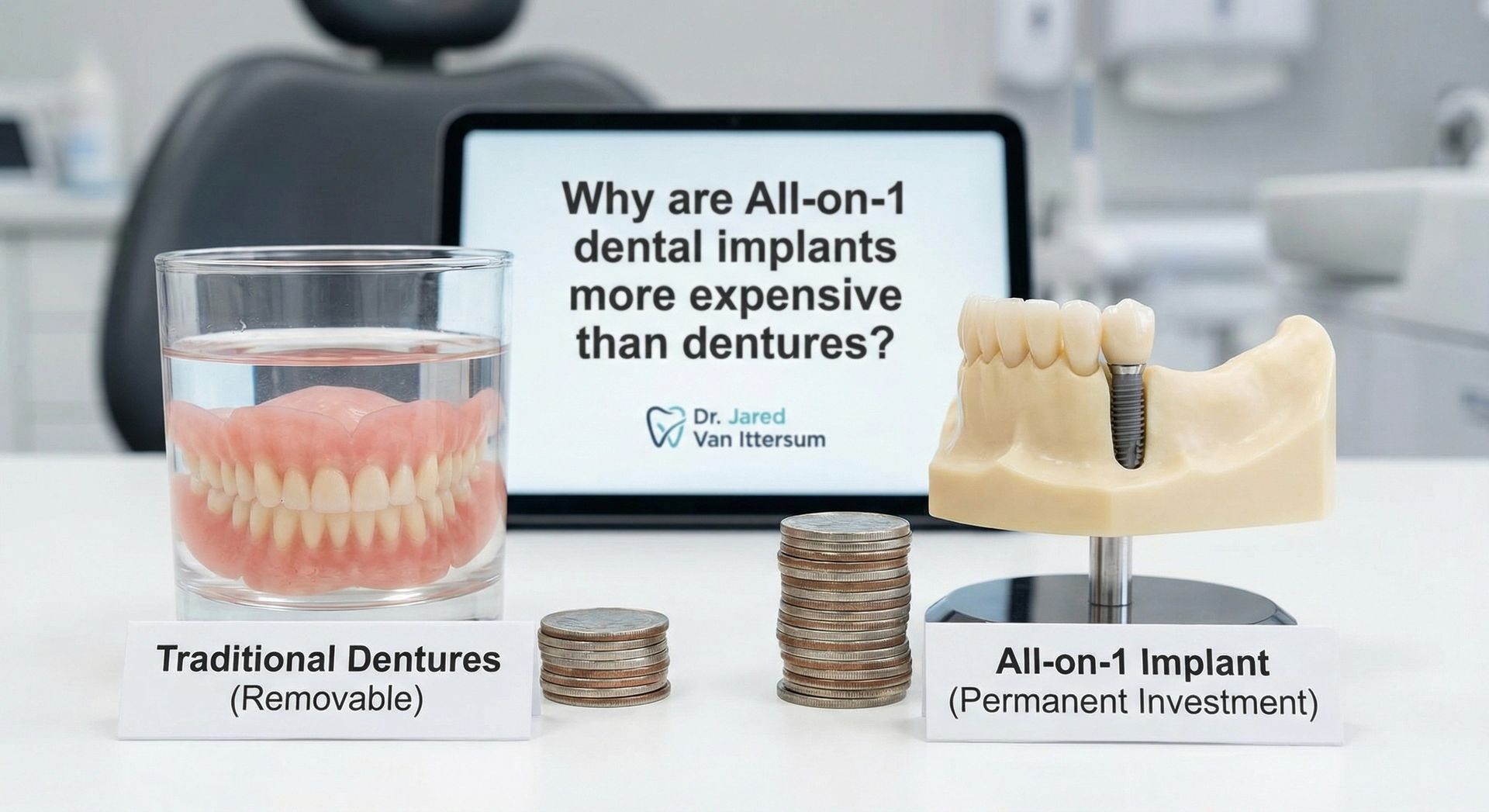
When dental implant failure occurs, replacement costs may include removal, bone grafting, re-insertion, and new prosthetics. Who ultimately pays depends on insurance coverage, practice policy, and manufacturer warranties. Some comprehensive dental insurance plans offer partial reimbursement for failed implants, especially if failure occurs within a set “warranty period. ” Individual practices often provide discounted rates or free corrections for failures within 1–3 years, but policies vary widely. At our practice, we provide a 25-year guarantee.
To minimize out-of-pocket expenses, patients should:
- Clarify terms of service, warranties, and insurance coverage before proceeding.
- Ask providers about written guarantees or coverage for early failures.
- Negotiate for extended coverage or discounted replacement procedures.
- Keep thorough records of all dental care and communications.
- Expert dental guidance and patient testimonials on reducing implant failure risk
People Also Ask: Your Top Questions on All-on-1 Implant Failure Rate Answered
How common is dental implant failure?
- Most studies estimate the general dental implant failure rate at 2% to 5% over several years, with All-on-1 implant systems showing similar or lower failure rates due to advancements in technique and patient screening.
Who pays when a dental implant fails?
- Responsibility depends on warranty, insurance, and practice policy—patients should clarify these details before treatment. Many practices offer partial coverage or discounted corrections for failed implants.
Where is the highest rate of implant failure?
- Higher failure rates are associated with poor bone quality (such as upper jaw placement), inadequate oral hygiene, and systemic health issues, with rates varying regionally based on practitioner experience and resources.
How long do all-in-one implants last?
- All-on-1 implants routinely last for 20 years or longer.
Frequently Asked Questions: All-on-1 Implant Failure Rate
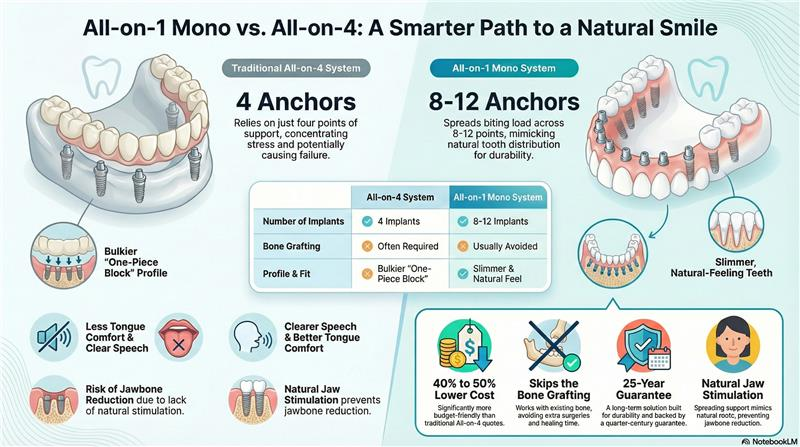
- Why are All-on-1 implant failure rates lower than traditional implants?
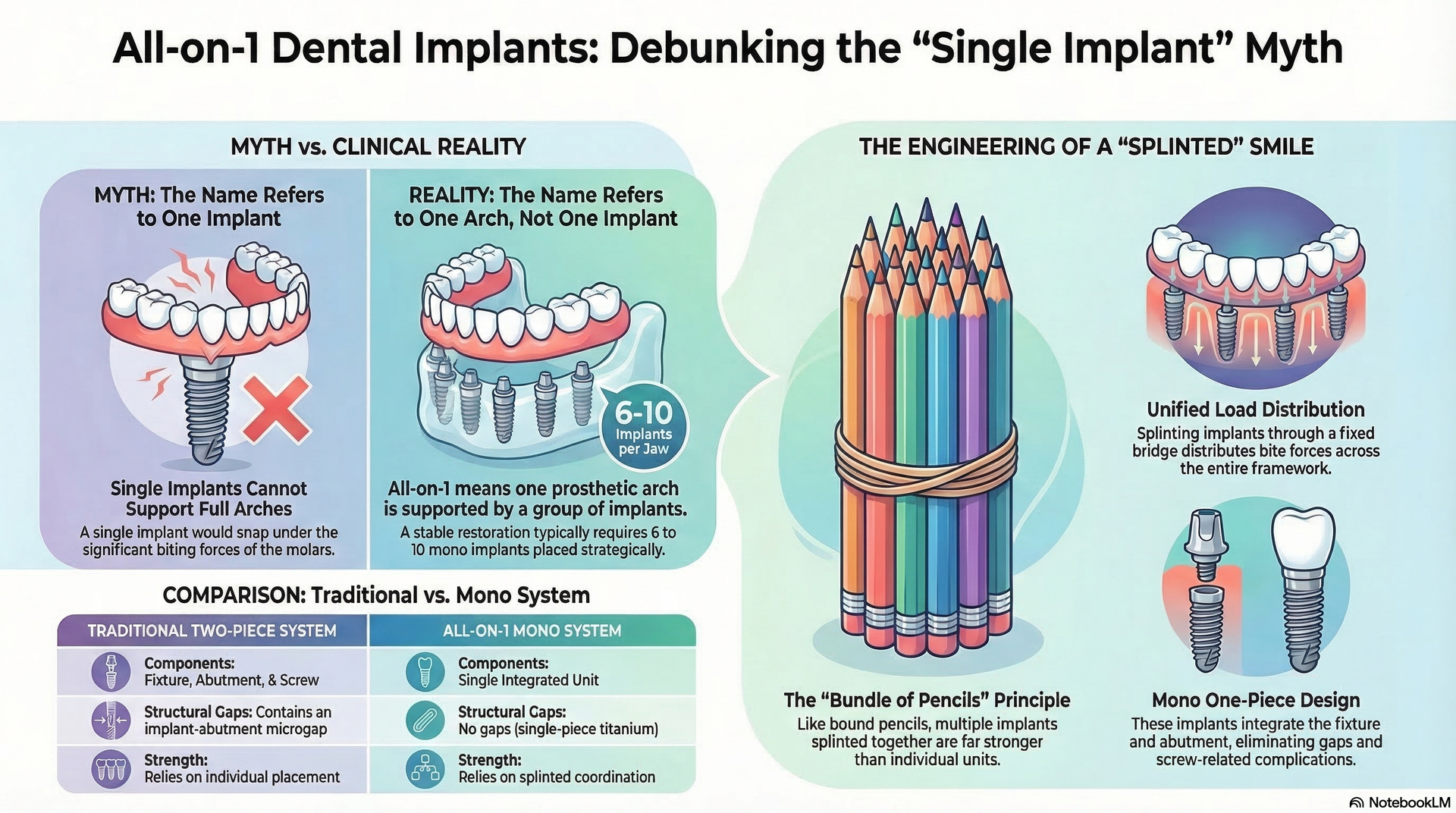
All-on-1 techniques use a single-piece implant and are inserted into the outer layer of bone, which provides additional support for the implant. Also, careful patient screening, strategic implant placement, and immediate loading protocols—factors that together reduce the risk of complications and improve implant integration, leading to lower observed failure rates.
- What is considered an implant failure?
An implant is considered failed if it becomes mobile, fails to integrate with bone, is associated with ongoing pain or infection, or requires removal at any stage after placement.
- Can bone loss after surgery lead to implant failure?
Yes, bone loss compromises implant stability and can be a leading cause of late failure. Regular dental checkups and good hygiene practices can help detect and prevent this risk early.
- What steps can I take post-surgery to reduce implant failure?
Keep up with professional cleanings, brush and floss daily, avoid smoking, and closely follow your dental team’s recommendations for recovery and maintenance. Promptly report any unusual symptoms for early intervention.
Key Takeaways on the Failure Rate of All-on-1 Implants
- All-on-1 dental implant systems have a very high success and survival rate.
- Failure rate remains low with proper patient selection and excellent oral care.
- Understanding failure risks and prevention strategies is key to long-term implant health.
Ready to Restore Your Smile? Schedule a Consultation to Discuss All-on-1 Implants
Take the first step toward a brighter, more confident smile by booking a personalized consultation with your local dental implant specialist. Discover why All-on-1 implants are one of the most reliable solutions for lasting oral health and function.
Recent Posts